STRESS FRACTURE
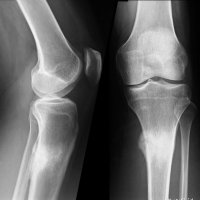
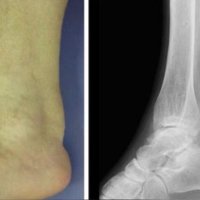
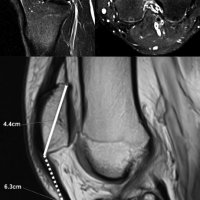
M, 38 y.o, marathon runner, with lump at proximal tibia and occasionally painful.
No history of trauma is noted.
Stress fractures refer to fractures occuring in bone due to a mismatch of bone strength and chronic mechanical stress placed upon the bone.
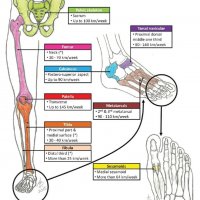
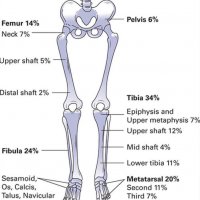
Stress fractures are far more common in the lower limb (-95%) than the upper limb.
High-risk sites of stress fractures usually are under tensile stresses and have poor vascularity
Plain radiographs have poor sensitivity (15-35%) in early-stage injuries, as positive findings may take months to appear.
MRI is the modality of choice for detecting stress fracture, and may also be useful for differentiating ligamentous/cartilagenous injury from bone injury.
EXTRASKELETAL OSTEOSARCOMA
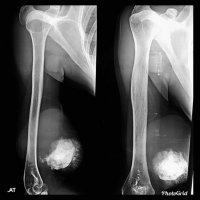
Extraskeletal Osteosarcoma is a rare mesenchymal malignant tumor that occurs in the retroperitoneum and soft tissue of extremities without any attachment to bone.
Most commonly occuring in individuals 40 to 80 years of age and male are more affected than females.
ESOS appears as soft tissue density with a variable amount of calcification which represents osteoid matrix formation, and is seen in -50% of cases.
Metastasis and local recurrence are quite common with ESOS, and this tumor is also insensitive to chemotherapy and radiotherapy.
The initial treatment strategy favors wide local excision of a primary tumor, including limb salvage surgery for extraskeletal osteosarcoma of the extremity.
ACHILLES TENDON XANTHOMAS
Achilles tendon xanthomas are painless soft tissue masses occurring most commonly at the distal one-third of the tendon and are usually bilateral and symmetrical.
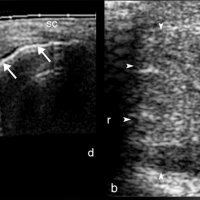
In plain radiograph, this condition appearas as soft tissue densities in the Achilles tendon.
Ultrasound reveals increased AP thickness of the tendon >7 mm in males and >6 mm in females, also loss of normal tendon appearance with multiple hypoechoic foci within the tendon.
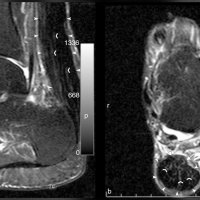
MRI shows focal thickening of the tendon with increased AP diameter, loss of the normal anterior concavity of the tendon with speckled appearance of the tendon, hyperintense on T1- and T2-weighted images.
BILATERAL HIP PAIN
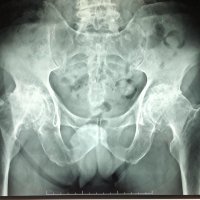
M, 77 y.o, with bilateral hip pain.
Anteroposterior pelvis radiograph reveals complete obliteration of bilateral hip joints space with associated marginal osteophyte, subchondral sclerosis and cyst formation, also deformity of femoral heads and acetabulum, in keeping with severe osteoarthritis of the hips.
An asphericity of the femoral heads with osseous “bump” formation at the anterolateral femoral head-neck junction just lateral to the physeal scar is also noted, consistent with cam deformity.
This asphericity leads to unwanted force transmission to the acetabulum during flexion and internal rotation, leading to wear and tear of the labrum dan cartilage, and subsequently resulting in degenerative joint disease.
Cam deformity is usually causes by a primary osseous variant of the head-neck junction, but it also can be the result of several known etiologies include malunion of a femoral neck fracture, slipped capital femoral epiphysis, developmental dysplasia of the hip, or Legg-Calve-Perthes’ disease.
Courtesy of Dr. dr. Elysanti Dwi Martadiani, Sp.Rad(K)
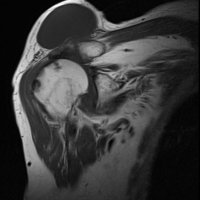
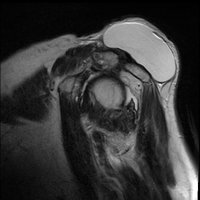
THE GEYSER SIGN IS A SUBCUTANEOUS PSEUDOTUMOR ABOVE THE ACROMIOCLAVICULAR JOINT
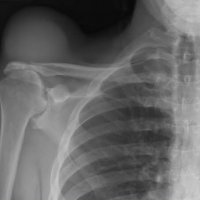
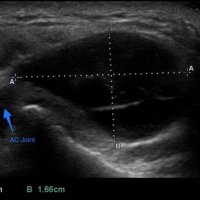
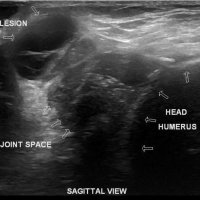
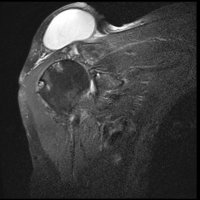
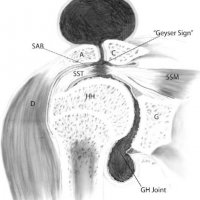
The geyser sign is a subcutaneous pseudotumor above the acromioclavicular joint, also known as AC joint cyst. The geyser sign is an infrequently encountered imaging sign that was originally described on conventional fluoroscopy-guided shoulder arthrography. The first case report of these cysts occuring in association with rotator cuff tears was made by Dr. Edward Craig in 1984, and again in 1986. The sign derives its name from its geyser-like appearance.
On physical examination, an AC joint cyst is a palpable fluid-filled mass. MRI scanning or a shoulder arthrogram should be obtained to evaluate the shoulder. Unenhanced MRI scans showing a large rotator cuff tear, a degenerated AC joint, and a large subcutaneous cyst adjacent to the AC joint is virtually patognomonic for the disease. Contrast administration on MR arthrogram will show the synovial fluid or intra-articular contrast extravasates from the glenohumeral joint into the subacromial bursa, into the AC joint, and then into an overlying cystic mass when a full-thickness rotator cuff tear is present, resembling a geyser spouting upwards.
Initial treatment is conservative and involves physical therapy along with aspiration. In patients with functional impairment or chronic shoulder pain who have failed conservative management, surgical treatment is recommended for both excision of the cyst and repair of the rotator cuff tear.
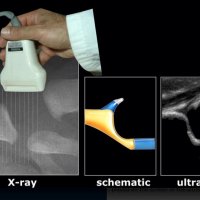
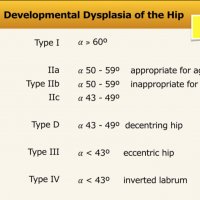
DEVELOPMENTAL DYSPLASIA OF THE HIP (DDH)
Developmental dysplasia of the hip (DDH) is one of the most common musculoskeletal problems in newborns. It results from an abnormal relationship of the femoral head to the acetabulum. The reported incidence of DDH varies between 1.5 and 20 per 1000 births, with a clear female predominance (M:F ratio ~1:8). DDH usually occurs from ligamentous laxity and abnormal position in utero. For some reason, the left hip is said to be more frequently affected. One-third of cases are affected bilaterally.
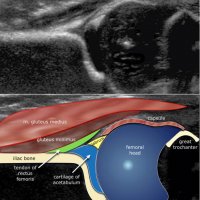
Ultrasound is the modality of choice for imaging assessment of DDH in the infant (<6 months) prior to ossification of the proximal femoral epiphysis. A lineair, high frequency probe is used and the focus is set at the acetabular edge. Once there is a significant ossification then x-ray examination is required.
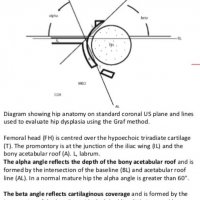
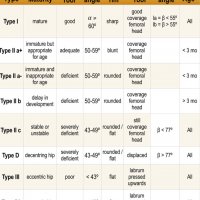
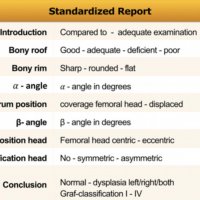
The Graf classification of hip dysplasia is mainly based on the morphology of the iliac bone, where we look at the shape of the acetabulum, the bony and cartilaginous acetabular rim, labrum and position of the femoral head, and also look at the coverage of the femoral head by the cartilage of the acetabulum and the labrum.
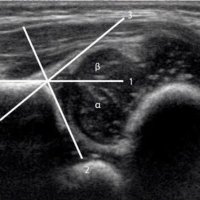
The alpha-angle, which is a measurement of the bony roof of the acetabulum, mainly determines the hip type. The normal value is greater than or equal to 60º. Note that up to the age of 3 months (13 weeks) an alpha angle below 60 degrees is acceptable.
The beta angle is formed by the vertical cortex of the ilium and the triangular labral fibrocartilage. The normal value is less than 77º but is only useful in assessing immature hips when combined with the alpha angle, to differentiate between type Ia and Ib (both normal hips) and between type IIc and type D.
Bony coverage represents the percentage of the femoral epiphysis covered by the acetabular roof. A value of >50% is considered normal.
Treatment varies from Pavlik bracing to surgical reduction and osteotomies depending on the age of the patient and the degree of dysplasia.
PATELLAR TENDON-LATERAL FEMORAL CONDYLE FRICTION SYNDROME
Patellar tendon-lateral femoral condyle friction syndrome, also known as Hoffa fat pad impingement syndrome, is a common cause of anterior knee pain in active individuals. It is thought to be due to patella maltracking or imbalance of the forces between medial and lateral vastus muscles causing impingement of the superolateral aspect of Hoffa fat pad between the inferior patella and the lateral femoral condyle.
Patients with Hoffa syndrome would present with acute or chronic sharp pain below the patella which is worsened by activities like walking, prolonged standing, wearing high heel shoes or any other activity that puts the knee into full extension. On examination, there may be swelling in the infrapatellar region, with point tenderness at the inferior pole of the patella.
The diagnosis is classically made with MRI and usually occult on radiography and CT. MRI findings include focal area of high T2 signal (edema) at the inferolateral aspect of the patellofemoral joint, within the superolateral portion of the infrapatellar fat pad. A cystic lesion can sometimes be found between the lateral femoral condyle and the lateral retinaculum. Associated findings include lateral patellar subluxation and patella alta (Insall-Salvati ratio greater than 1.2) which are found in around 90% of cases. Conservative treatment is usually successful, although full recovery may take time.